Responding to Opioid Overdose

**IF SOMEONE IS EXPERIENCING A MEDICAL EMERGENCY, CALL 911 IMMEDIATELY**
Is someone overdosing? The most important thing is to act right away!
It is rare for someone to die immediately from an overdose – it is usually a slowish process that takes anywhere from a few minutes to a few hours. When people survive, it’s because someone was there to respond.
If someone is overdosing, they will be 1) not breathing and 2) not responsive. Below are the immediate steps you want to take in the event of an opioid overdose.
If someone is not breathing (skin turning blue/gray, pinpoint pupils, deep gurgling sound) and not responsive, follow these steps. You’ll find more info on each of these steps below. You can also see a video from NHRC’s DOPE Project team here, which breaks down how to recognize and reverse an overdose as well as aftercare steps.
STEP 1. Stimulate them awake by yelling their name and administering a hard sternum rub to the chest plate.
STEP 2. If you have naloxone/Narcan, use it. Administer one dose every 2-3 minutes.
- Injectable: Draw up entire vial and inject into thigh muscle (must be muscle’ed to work)
- Nasal: Stick the device all the way up one nostril and click the plunger, make sure the device is inserted fully (medication will absorb through the sinuses)
STEP 3. Call 911, explain someone is not responsive and not breathing
STEP 4. Provide rescue breathing
- Get the person on their back, tip their head back to straighten the airway, pinch their nose, put your mouth over theirs and form a seal, one breath every five seconds
STEP 5. When the person starts to breathe regularly on their own, roll them into a recovery position on their side
STEP 6. Be gentle with them and yourself afterwards!
Assessment & Stimulation
If you are unsure if the person is overdosing, there are obvious signs you can assess.
- Is the person breathing?
- Is the person responsive?
- Do they answer when you ‘shake and shout’ their name?
- Can the person speak?
- How is their skin color (especially lips and fingertips)?
Stimulate the person
If the person is unconscious or in a heavy nod, try to stimulate them awake through verbal and/or physical stimulation.
Verbal Stimulation
Call their name and/or say something that they might not want to hear, like “I’m going to call 911” or “I’m going to give you naloxone.”
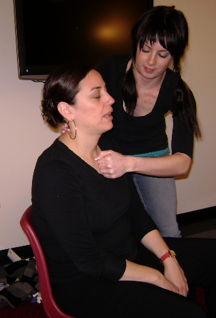
Physical Stimulation
If this does not work, try to stimulate him or her with pain to wake them up.
- rub your knuckles into the sternum (the place in the middle of your chest where your ribs meet)
- rub your knuckles on their upper lip.
- pinch the back of their arm.
If this causes the person to wake up try to get him or her to focus. Can they speak to you? Check their breathing. If this is shallow or the person tells you they have shortness of breath, or chest tightness call 911. Continue to monitor them, especially the breathing and pulse and try to keep him or her awake and alert.
If the person DOES NOT respond to stimulation and remains unconscious or the condition appears to get worse, do NOT try a different or alternative form of stimulation. Treat this as an emergency and call for help!
2. Call for Help!
It is recommended you call 911 in the case of an overdose because it is important to have trained medical professionals assess the condition of the overdosing person.
Even though naloxone can fix the overdose, there may be other health problems going on. Also, people who survive any type of overdose are at risk of experiencing other health complications as a result of the OD, such as pneumonia and heart problems. Getting someone to be checked out by a medical professional is an important part of reducing the harms associated with overdosing.
What to Say to 911
What to say when calling 911 depends on the local emergency response to overdoses. In every community, it is important to report that the person’s breathing has slowed or stopped, they are unresponsive, and give the exact location. If naloxone was given and it did not work, tell the dispatcher this. In many communities, the police respond along with the ambulance to all 911 calls. In some communities, when the police respond they do not arrest the bystander or victim at the scene of an overdose. However, in other places the police do arrest people at the scene of the overdose, and have been known to charge people with everything from drug possession, to manslaughter (if the overdosing person dies and the bystander is proven to be the supplier of drugs). The fear of arrest and police involvement is substantial. Agencies should try to learn from participants what the real risk is and work with police and emergency personnel to address the fear of arrest and police involvement.
When making the call:
- Tell the dispatcher exactly where you and the overdosing person are. Give them as much information as possible so that they can find you (i.e. 3rd floor, or in the bathroom).
- Avoid using words like drugs or overdose—stick to what you see: “Not breathing, turning blue, unconscious, non-responsive, etc.” This makes the call a priority.
- When the paramedics arrive, tell them what you know about what drugs the person may have been using—as much information as possible. If the paramedics suspect opioids, they will give the victim an injection or intranasal dose of naloxone.
- Keep loud noise in background to a minimum—if it sounds chaotic, they will surely dispatch police to secure the scene and protect the paramedics
Put the Person in the Recovery Position
If you have to leave the person at all, even for a minute to phone 911, make sure you put them in the recovery position.
- Lay the person slightly on their side
- Bend their knee
- Turn their face to the side.
- This will help to keep their airway clear and prevent them from choking on their own vomit if they begin to throw up.

If Calling 911 is Not an Option
If calling 911 is not an option (some people will not call), it is important to make some alternate plans if your rescue attempts are not working. Can someone else in the vicinity call? Could you provide rescue breathing, naloxone, and put the person in the recovery position and then leave to alert someone to call, even a passerby? Leave the person where they can be found, with doors unlocked and/or open.
Remember, doing something is better than doing nothing.
3. Administer Naloxone
Naloxone is a life-saving medication that counters the effects of an opioid overdose. It is available as both a nasal spray and an injectable.
REMEMBER! Naloxone only works if there are opioids involved with the OD. It cannot reverse an OD of cocaine, speed, benzos, alcohol or other non-opioid based drugs.
How to Give Nasal Spray Naloxone
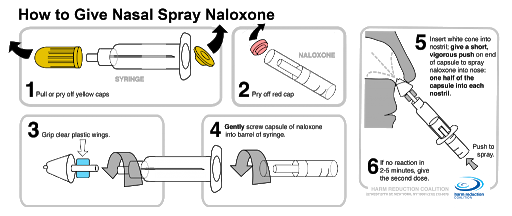

- Do rescue breathing for a few quick breaths if the person is not breathing.
- Affix the nasal atomizer (applicator) to the needleless syringe and then assemble the glass cartridge of naloxone (see diagram).
- Tilt the head back and spray half of the naloxone up one side of the nose (1cc) and half up the other side of the nose (1cc).
- If there is no breathing or breathing continues to be shallow, continue to perform rescue breathing for them while waiting for the naloxone to take effect.
If there is no change in 2-3 minutes, administer another dose of naloxone and continue to breathe for them. If the second dose of naloxone does not revive them, something else is wrong—either it has been too long and the heart has already stopped, there are no opioids in their system, or the opioids are unusually strong and require more naloxone (can happen with fentanyl, for example).
How to Administer Injectable Naloxone
Injectable naloxone comes packaged in several different forms- a multi dose 10 mL vial and single dose 1mL flip-top vials with a pop off top. With all formulations of naloxone, it is important to check the expiration date and make sure to keep it from light if it is not stored in a box. If someone has an injectable formulation of naloxone, all of the steps in recognizing and responding to an overdose are the same except how to give the naloxone. To use injectable naloxone:
- Do rescue breathing for a few quick breaths if the person is not breathing.
- Use a long needle: 1 – 1 ½ inch (called an IM or intramuscular needle)- needle exchange programs and pharmacies have these needles.
- Pop off the orange top vial.
- Draw up 1cc of naloxone into the syringe 1cc=1mL=100u.
- Inject into a muscle – thighs, upper, outer quadrant of the butt, or shoulder are best.
- Inject straight in to make sure to hit the muscle.
- If there isn’t a big needle, a smaller needle is OK and inject under the skin, but if possible it is better to inject into a muscle.
- After injection, continue rescue breathing 2-3 minutes.
If there is no change in 2-3 minutes, administer another dose of naloxone and continue to breathe for them. If the second dose of naloxone does not revive them, something else may be wrong—either it has been too long and the heart has already stopped, there are no opioids in their system, or the opioids are unusually strong and require more naloxone (can happen with Fentanyl, for example).
Once naloxone has been delivered and if the person is not breathing, continued rescue breathing is important until help arrives.
Naloxone only lasts between 30 – 90 minutes, while the effects of the opioids may last much longer. It is possible that after the naloxone wears off the overdose could recur. It is very important that someone stay with the person and wait out the risk period just in case another dose of naloxone is necessary.
Also, naloxone can cause uncomfortable withdrawal feelings since it blocks the action of opioids in the brain. Sometimes people want to use again immediately to stop the withdrawal feelings. This could result in another overdose. Try to support the person during this time period and encourage him or her not to use drugs for a couple of hours.
IMPORTANT!
If a victim is not responsive to stimulation, not breathing, and has no pulse after receiving naloxone and rescue breathing, then the victim needs cardiopulmonary resuscitation (CPR) via a trained bystander and the emergency medical system. Call 911!
4. Perform Rescue Breathing or Chest Compressions
For a person whose breathing is severely impaired, rescue breathing or chest compressions is one of the most important steps in preventing an overdose death. When someone has extremely shallow and intermittent breathing (around one breath every 5-10 seconds) or has stopped breathing and is unresponsive, rescue breathing should be done as soon as possible because it is the quickest way to get oxygen into someone who has stopped breathing.
If you are performing rescue breathing, you are getting much needed air into someone’s body who will die without it. The difference between survival and death in an opioid overdose depends on how quickly enough oxygen gets into the person’s body.
These are the steps for rescue breathing:
- Place the person on their back.
- Tilt their chin up to open the airway.
- Check to see if there is anything in their mouth blocking their airway, such as gum, toothpick, undissolved pills, syringe cap, cheeked Fentanyl patch (these things have ALL been found in the mouths of overdosing people!). If so, remove it.
- Plug their nose with one hand, and give 2 even, regular-sized breaths. Blow enough air into their lungs to make their chest rise. If you don’t see their chest rise out of the corner of your eye, tilt the head back more and make sure you’re plugging their nose.
- Breathe again. Give one breath every 5 seconds.

You may have heard that recent CPR guidelines recommend “hands-only CPR,” or only chest compressions instead of rescue breathing and chest compressions. These guidelines are for layperson response to cardiac arrest, and NOT overdose. It is still recommended that you perform rescue breathing for an overdose, where the primary issue is respiratory depression, and not cardiac arrest.If you are alone with the overdosing person, follow these steps and give the person a few breaths and then put them in the Recovery Position and go get your naloxone kit. If there is more than one of you there to respond to the overdose, DIVIDE DUTIES – have one of you do rescue breathing and the other can go get the naloxone kit. If you don’t have a naloxone kit, continue rescue breathing until help (i.e. the ambulance) arrives. If there’s more than one person present, take turns rescue breathing – it can be exhausting.
5. Aftercare
Because naloxone blocks opioids from acting, it is possible that it can cause withdrawal symptoms in someone that has a habit, daily opioid pain medication use or other opioid tolerance. Therefore, after giving someone naloxone he or she may feel dopesick and want to use again right away. It is very important that one does not use drugs again until the naloxone wears off so that a re-overdose does not occur.
Bystanders who use naloxone often report that it works immediately, however it may take up to 8 minutes to have an effect. Naloxone’s effect lasts for about 30 to 90 minutes in the body. Because most opioids last longer than that, the naloxone may wear off before the effects of the opioids wear off and the person might go into an overdose again. Naloxone administration may be repeated without harm if the person overdoses again. In addition, if the person uses more heroin or opioids when there is still naloxone in the system, he or she may not feel it at all – naloxone will knock it out of the opioid receptors and the person will have wasted their drugs.
The likelihood of overdosing again depends on several things including:
- How much drug was used in the first place and the half-life of the drug(s) taken
- How well the liver works to process things; and
- If the person uses again.
If the person cannot walk and talk well after waking up, then it is very important that they are taken to the hospital. If possible, stay with the person for several hours keeping them awake.
